The Birth Story Loop: When “Healthy Baby, Healthy Mom” Isn't Enough
Birth trauma isn't just about what happened in the delivery room—it’s about the mental 'loops' that follow. Dr. Erin Cook explores the intersection of birth trauma and OCD, explaining how a 'clinical emergency' can trigger chronic rumination. Learn how Narrative Therapy and ERP provide a gold-standard path to recovery for postpartum parents.
Sarah had always been a planner. From her college applications to her wedding seating chart, her life was a series of well-executed visions. When she got pregnant, she approached motherhood with that same intentionality. She spent months curating the perfect nursery, researching breast pumps, and eventually, crafting a birth plan that felt like a sanctuary.
She imagined the dim lighting, the specific playlist, and the freedom to move. She was even "rational" about the possibility of a C-section: “As long as we’re both happy and healthy, who cares how the baby comes?” she’d tell herself.
But when Sarah went into labor at 35 weeks, the plan didn't just change—it evaporated.
Suddenly, she wasn't in a dimly lit room with a birth ball; she was hooked to monitors in a sterile high-risk unit. Her blood pressure soared. She was placed on a magnesium drip—a medication that felt like a heavy, searing fog settled over her brain. Her regular doctor was out of town, and the on-call physician seemed to view her birth plan as a list of suggestions rather than her deeply held values.
In that room, the medical team saw a “clinical emergency” to be managed, but Sarah felt like a person being erased. She felt like a vessel for a baby rather than a participant in her own life. That loss of voice—that moment where her “No” or her “Wait” was ignored—became the sharpest edge of the experience.
The Birth of the Loop
A week later, Sarah was home. Her daughter was healthy, and the beautiful nursery was finally in use. But Sarah’s mind was still in that hospital room.
Even though the physical "outcome" was a success, Sarah found herself stuck in what we call the Birth Story Loop. Every time she looked at her daughter, her brain would pivot:
“What if I had rested more in those last few weeks?”
“What if I had advocated harder when the doctor mentioned the induction?”
“Did I fail because I didn't push longer?”
Every time a "perfect" birth announcement popped up on her Instagram feed, she felt a physical pang of jealousy, followed immediately by a wave of shame. She felt like a "bad mom" for not being able to celebrate others, not realizing her brain was simply triggered by the contrast between their agency and her trauma.
Why the Brain Loops: The Unfinished Puzzle
For high-achievers like Sarah, the brain treats a traumatic or disappointing birth like an unsolved puzzle. Because of the magnesium fog and the sheer adrenaline of the emergency, Sarah’s brain didn't get to "record" the birth in a linear way.
It’s like a book with five missing pages in the middle. Her brain keeps looping back to those pages, trying to fill in the blanks of what happened while she was "out of it," hoping that "certainty" will finally bring peace.
In reality, this is rumination—a mental compulsion. The more Sarah "checks" her memories or asks for reassurance from her husband ("Do you think the doctor waited too long?"), the more her brain stays in emergency mode. She isn't processing the birth; she’s re-traumatizing herself through the loop.
How We Break the Loop in Therapy
At Red Elm, we help parents break the loop using a two-pillar approach:
1. Narrative Therapy: Reclaiming the Story We work to externalize the "failure." Sarah didn't fail her birth; she navigated a medical event that went off-script. We move from the toxic positivity of "at least everyone is okay" to the emotional truth of "this was scary, and I am allowed to grieve the experience I didn't get." We help you integrate the disappointment so it becomes a part of your history, rather than a shameful secret.
2. ERP: Stopping the Compulsions Exposure and Response Prevention (ERP) is the "gold standard" for the anxiety and OCD that often follows a difficult birth.
The "Response Prevention": We identify the reassurance-seeking (the googling, the constant asking of a partner) and practice sitting with the discomfort of not knowing for sure.
The "Exposure": We might write out the "scariest version" of the birth story and read it together until the "shiver" it sends down your spine begins to habituate.
Beyond “Healthy”
If you find yourself stuck in a birth story loop, know that your disappointment isn't ungratefulness. It is a sign that your brain is trying to make sense of a moment where you lost your agency.
Therapy isn’t about changing what happened in that hospital room. But we can stop the birth from "happening" to you every single day in your head. It’s time to reclaim your energy for the life you’re building now.
Reach out now to stop the birth story loop.
About the Author
Dr. Erin Cook is a clinical psychologist and co-founder of Red Elm Psychotherapy, a Virginia-based practice specializing in perinatal mental health and OCD.
She works with women navigating the complexities of pregnancy, postpartum, and early motherhood—specializing in those moments when anxiety or intrusive thoughts feel overwhelming or out of character. Her approach to treating birth trauma is collaborative, thoughtful, and grounded in helping clients understand the "why" behind their brain’s loops so they can finally feel less alone in their experience.
When Insight Isn’t Enough: Why OCD Still Feels So Convincing
You know the thought is irrational, yet five minutes later you're back in the loop. The problem isn't a lack of logic—it’s an excess of it. Discover why your intelligence is being weaponized against you and how to finally 'drop the rope' in the mental tug-of-war.
You know the thought doesn’t make sense. You’ve analyzed it from every angle. You’ve checked the facts. You’ve reassured yourself.
Maybe you’ve even had a moment where you thought: “Okay. This is definitely Obsessive-Compulsive Disorder (OCD).”
And then five minutes later, the anxiety comes rushing back. Your stomach drops. The doubt feels real again. And suddenly you’re back in the loop trying to solve it one more time.
If this happens to you, you are not failing at being rational. In fact, many people with OCD are exceptionally intelligent, analytical people. That’s part of what makes OCD so convincing.
OCD Turns Intelligence Against You
In most areas of life, thinking harder helps. Being responsible and paying attention to details are traits that probably helped you succeed in school, work, or parenting.
But OCD hijacks those same strengths. Instead of using your mind to solve real-world problems, OCD pulls you into impossible ones:
“What if I secretly meant that thought?”
“What if I’m missing something important?”
“What if I can never be fully certain?”
At some point, the thinking itself becomes the compulsion. Not because you’re irrational, but because your brain is desperately trying to make the anxiety stop.
What Mental Compulsions Actually Look Like
A lot of people imagine OCD as visible checking or hand washing. But many compulsions happen entirely inside your head. From the outside, you may look calm. Inside, you are exhausted.
You might spend hours replaying conversations, reviewing memories, or checking whether a feeling "feels true." Depending on what you value most, these loops can take many forms:
Relationship OCD (ROCD): Constantly analyzing your partner or your feelings to "prove" you are in the right relationship.
Perinatal OCD: Intrusive, terrifying thoughts about the safety of your baby and the constant mental checking that follows.
Scrupulosity: A painful loop of moral or religious doubt, where you feel you must constantly "fix" your standing with God or your conscience.
The OCD Cycle: The universal engine that keeps all these themes running on a loop.
Why Insight Alone Doesn’t Stop OCD
One of the most painful parts of OCD is that you likely already know your fears are irrational. Insight is not the problem. You can understand OCD intellectually and still feel trapped by it emotionally because OCD is not a logic problem; it’s an alarm system problem. Your brain sends out a false signal of danger, and your mind works overtime to explain why the danger feels so real. Unfortunately, the more seriously you treat the thought—by analyzing or researching it—the more important your brain believes it must be.
The Tug of War
Imagine you are standing at the edge of a canyon. On the other side is a monster representing your intrusive thoughts. Between you is a rope.
The moment an intrusive thought appears, the monster yanks the rope. Instinctively, you pull back. You try to prove the thought wrong or get certainty. But the harder you pull, the more consumed you become by the fight. Soon, your entire life revolves around the rope.
ERP Is About Leaving the Fight
This is where Exposure and Response Prevention (ERP) changes things. ERP is not about proving the intrusive thought false or "thinking more rationally."
ERP helps you learn how to stop engaging with the struggle altogether. Whether you are dealing with harm OCD, contamination fears, or the constant "background noise" of uncertainty, the goal is not to defeat the monster; the goal is to stop organizing your life around it.
What “Dropping the Rope” Looks Like:
ERP teaches you to practice allowing uncertainty to exist.
That might mean:
Allowing a scary thought to stay without analyzing it.
Resisting the urge to mentally review your day.
Noticing anxiety without trying to "neutralize" it.
At first, this feels deeply uncomfortable. It feels irresponsible to let the "what if" go unanswered. But over time, your brain learns the truth: The thought itself was never the danger.
Here is the problem with doing this alone: Your brain is convinced that the rope is the only thing keeping you safe. It tells you that if you let go, the monster wins, or something terrible will happen. Dropping the rope feels like an act of negligence.
This is one of my main roles in guiding clients through [Exposure and Response Prevention (ERP)]: to stand at the edge of that canyon with you. I help you tolerate the "itch" to pull back until your brain finally learns that the monster can’t actually cross the canyon—whether you hold the rope or not.
A 30-Second Exercise: Practice the Pause
You don’t have to drop the rope forever right this second. Today, just practice delaying the pull.
Next time you feel that jolt of anxiety and the urge to "figure it out" or check a memory hits:
Acknowledge the rope: Say to yourself, "OCD just threw me the rope."
Set a timer for 30 seconds: Do not analyze, do not Google, and do not replay the memory for just thirty seconds.
Feel the tension: Notice the discomfort in your body without trying to fix it.
Even if you go back to the loop after those 30 seconds, you’ve just proven something huge: You are the one in control of your hands, even when the anxiety is loud.
You Don’t Need More Insight. You Need a Different Response.
Many people who reach out for OCD treatment are already highly self-aware. They’ve read the articles; they can explain the cycle better than anyone. But they still feel trapped.
Recovery doesn't happen through more analysis. It happens through learning a different relationship with fear.
OCD Therapy in Virginia
I work with adults struggling with OCD, intrusive thoughts, rumination, and mental compulsions using evidence-based ERP therapy.
Together, we focus on helping you step out of the exhausting mental loops so you can spend less time trapped in your head and more time fully engaged in your life.
Ready to drop the rope?
About the Author
Dr. Niles Cook is a licensed clinical psychologist and co-founder of Red Elm Psychotherapy. He specializes in helping high-achieving adults and professionals who are exhausted by the "intelligence trap"—where the same analytical skills that made them successful are now being used by OCD to keep them stuck in cycles of doubt.
Using Exposure and Response Prevention (ERP), Dr. Cook provides a structured, no-nonsense path for clients to stop over-analyzing their lives and start living them. His approach is direct, collaborative, and designed for those who need more than just insight—they need a different way to respond to fear.
Dr. Cook provides specialized telehealth therapy across the state of Virginia.
Note: This content is educational and does not constitute medical advice or a therapist-client relationship. If you are in a crisis, please call 988 or go to the nearest emergency room.
Why Your Relationship Feels Different After a Baby — Especially When Anxiety or OCD Is Involved
Some couples don’t fight more after a baby.
Instead, things start to feel… off.
You’re functioning. You’re getting through the day. But something in the relationship feels quieter, more distant—and harder to explain.
For many high-functioning women, anxiety and intrusive thoughts don’t just stay internal. They subtly reshape how you show up with your partner.
Some couples don’t fight more after they bring their baby home. They aren’t having dramatic arguments or obvious problems. But somewhere between the diapers and the sleepless nights, something shifts.
Things don’t feel bad—just… off.
There’s a little more distance. A little less ease. You might find yourself feeling less connected to the person you just started a family with—and you aren't entirely sure why.
For many women, this shift is compounded by anxiety, intrusive thoughts, or patterns that feel difficult to explain—especially during pregnancy or the postpartum period. If you’re having thoughts that feel disturbing, out of character, or hard to talk about—you are not alone. This is something we treat often at Red Elm Psychotherapy.
When Anxiety Becomes a Third Partner
When anxiety or OCD is present, the relationship often becomes one of the primary places it gets expressed. This can show up as general anxiety, intrusive thoughts, or more defined OCD patterns—but the impact on the relationship often feels the same.
Anxiety is driven by a need for certainty. In a partnership, that often translates into:
Constant Scanning: Checking your partner’s face or tone for signs of frustration, boredom, or distance.
Reassurance Seeking: Asking the same questions repeatedly to soothe a “sticky” thought (e.g.,“Is the baby breathing?” or "Are we okay?" ).
Over-Responsibility: Feeling like you must carry the entire emotional or physical load to prevent something “bad” from happening.
Hypersensitivity: Interpreting a neutral moment—like a quiet dinner or a short text—as a sign that the relationship is failing.
These thoughts are unwanted, distressing, and often completely out of character. They are not a reflection of your intentions or the quality of your bond. We go into more detail about how this pattern works on our Perinatal OCD page.
Sometimes, the anxiety begins to focus on the relationship itself. This is often referred to as Relationship OCD (ROCD), where “sticky” thoughts lead you to constantly question your partner’s “rightness” or search for flaws as a way to reach a certainty that doesn’t exist.
The Reassurance Loop: The Unwitting Accomplice
In high-functioning couples, partners are often incredibly kind and helpful. However, that kindness can unintentionally feed the anxiety.
In the world of OCD, this is called accommodation—when a partner’s well-intentioned efforts to reduce your distress actually keep the anxiety cycle spinning. Many people feel ashamed of how much reassurance they need and worry about "burdening" their partner.
A partner may provide reassurance, engage in repetitive “what-if” conversations, or try to become the "solution" to intrusive thoughts. The relationship starts to function as a tool for resolving anxiety. It works briefly, but the relief never lasts. Over time, this creates a painful cycle of tension, resentment, and loneliness—even when you’re sitting right next to each other.
The High-Functioning Mask
For many of the couples we see in Vienna and across Northern Virginia, everything looks fine from the outside. You are showing up. You look responsible. You are getting the job done.
You may be caring for a baby, managing a household, or returning to work—all while internally feeling overwhelmed or disconnected. But behind closed doors, there can be a deep sense of isolation. You aren’t “bad at communicating”—you’re navigating a system under sustained strain.
It’s Not Broken—It’s Under Strain
If this feels familiar, it doesn’t mean you picked the wrong partner or that your relationship is broken. It often means your relationship has been pulled into a cycle of anxiety.
The solution isn’t simply to “communicate better.” It’s understanding how you relate to each other through the lens of anxiety—and how certain patterns, even the ones born out of love, can keep both of you stuck.
How Therapy Helps
Therapy can help separate the anxiety from the relationship. Through structured, evidence-based approaches—including Exposure and Response Prevention (ERP) when appropriate—treatment focuses on:
Separating the anxiety from the person: Understanding that intrusive thoughts are not a reflection of who you are.
Reducing reassurance loops: Learning how to support each other without reinforcing the cycle.
Rebuilding steadiness: Moving away from reactive patterns and back toward the values that brought you together.
You don’t have to keep feeling "off." Understanding the pattern is often the first step toward feeling more like yourselves again.
Ready to Take the Next Step?
If your anxiety feels constant, intrusive, or difficult to step out of—especially during pregnancy or after having a baby—it may be more than something to simply "push through."
We specialize in helping women navigate postpartum anxiety, intrusive thoughts, and OCD. We use structured, evidence-based treatment designed to help you step out of the loop and feel more like yourself again.
We offer in-person sessions in Vienna, VA and work with clients across Virginia via telehealth, including McLean, Arlington, and the surrounding Northern Virginia area.
About the Author
Dr. Erin Cook, PsyD is a licensed clinical psychologist and co-founder of Red Elm Psychotherapy, a Virginia-based practice specializing in perinatal mental health and OCD. She works with women navigating pregnancy, postpartum, and early motherhood—particularly when anxiety or intrusive thoughts feel overwhelming or out of character.
Scrupulosity OCD: Why You Feel Like a Bad Person (Even When You’re Not)
“What if I’m actually a bad person and just don’t realize it?”
Scrupulosity OCD often sounds like this—and the more you try to figure it out, the more stuck you feel.
To others, you’re the responsible one. Thoughtful. Conscientious. Someone who cares deeply about doing the right thing.
But internally, it feels very different.
Your mind won’t stop asking:
Did I just lie?
Did I accidentally hurt someone?
What if I’m actually a bad person and don’t realize it?
You replay conversations. You analyze your intentions. You look for a feeling—some indication—that you’re “okay.”
And it never quite lands.
And even asking these questions can feel uncomfortable—like maybe it says something about who you are.
If your mind feels like a constant courtroom—evaluating, questioning, trying to reach a verdict—this may be Scrupulosity OCD, a specific subtype of OCD centered on morality, responsibility, and fear of being a bad person.
What Scrupulosity OCD Actually Is
Scrupulosity OCD is a form of obsessive-compulsive disorder (OCD) where intrusive doubts attach to morality, ethics, or religion.
At its core, this isn’t a problem with your values—it’s how your brain is responding to doubt about them.
Most people can tolerate some ambiguity about whether they handled something perfectly. They can think, “That might not have been ideal,” and move on.
OCD doesn’t allow that.
It demands something impossible:
“I need to know for sure that I am a good person.”
And because that kind of certainty doesn’t exist, the doubt never resolves.
What It Looks Like in Real Life
Scrupulosity OCD often looks like “being a good person”—just taken to a painful extreme. These patterns aren’t personality traits—they’re compulsions, attempts to reduce anxiety and feel certain.
You might notice:
Mentally replaying interactions to make sure you didn’t say something wrong or misleading
Compulsive confession or reassurance-seeking (“I need to tell them what I thought just in case”)
Over-apologizing for things that didn’t actually harm anyone
Internal checking (“Do I feel like a good person right now?”)
Decision paralysis around “ethical” choices (even small ones)
Researching or analyzing to prove you did the “right” thing
This can also show up in relationships, where doubt and responsibility feel especially high.
The intention is to feel certain.
The result is the opposite.
When Scrupulosity OCD Shows Up in Sexuality and the Body
For some individuals—especially those with a religious or high-moral framework—scrupulosity OCD extends into questions about sexuality, purity, and whether something is “right” or “wrong” in intimate relationships.
This can look like:
Persistent doubts about whether sexual thoughts, desires, or behaviors are immoral or “sinful”
Mentally reviewing intimate experiences to determine if something crossed a line
Seeking reassurance (from a partner, internally, or from a religious framework) about whether something was “okay”
Avoiding intimacy due to fear of doing something wrong
Feeling intense guilt, anxiety, or “moral distress” during or after sexual experiences
Over time, this doesn’t just stay in your thoughts—it can begin to affect the body.
Clinically, we often see:
Increased muscle tension, particularly in the pelvic floor
Difficulty relaxing during intimacy
Pain with sex that is worsened by anxiety and hypervigilance
A reinforcing cycle where physical discomfort increases fear, and fear increases physical tension
This isn’t just about beliefs or a lack of information.
It’s OCD attaching to something deeply meaningful and trying to eliminate uncertainty—using both the mind and body to do it.
This is an area where collaborative care can be especially important. When anxiety, guilt, or intrusive thoughts are contributing to muscle tension, pain, or difficulty with intimacy, working across disciplines can make a real difference.
We often coordinate care with providers supporting reproductive, sexual, or physical health to address both the psychological and physical patterns at the same time. Addressing one without the other often leaves the cycle intact.
The OCD Loop
Like all forms of OCD, scrupulosity follows a predictable cycle:
The Thought:
“What if I did something wrong?”
The Anxiety:
A surge of guilt, dread, or moral discomfort
The Compulsion:
Replaying, confessing, apologizing, researching, checking
The Relief:
Temporary—brief, incomplete
The Return of Doubt:
“But what if that wasn’t enough?”
The more you try to prove you’re a good person, the more uncertain you feel.
If this cycle feels familiar, you can read more about how OCD reinforces itself here.
Why Scrupulosity OCD Gets Missed
Scrupulosity OCD is often overlooked because the content of the thoughts sounds reasonable.
Who wouldn’t want to be honest, ethical, or kind?
Because of this, these patterns are often reinforced instead of recognized as OCD. You might even be praised for being conscientious or thoughtful.
But there’s an important difference between values and OCD:
Values guide behavior
OCD demands certainty and creates distress
This isn’t about becoming a better person or getting it exactly right. It’s about a brain that won’t let uncertainty settle.
Why This Can Feel So Distressing
For many people, this isn’t just anxiety—it feels like something deeper.
It can feel like:
“What if this means something about who I am?”
“What if other people would see me differently if they knew?”
“What if I can’t trust myself?”
That’s part of what makes scrupulosity OCD so painful.
It doesn’t just create doubt—it targets your sense of identity.
What Scrupulosity OCD Is NOT
It’s not:
Just being conscientious or thoughtful
A sign that you’re actually doing something wrong
A moral or character flaw
Something you can solve by thinking harder or trying to be “better”
If anything, people with scrupulosity tend to hold themselves to exceptionally high internal standards.
How ERP Therapy Treats Scrupulosity OCD
The way out of Scrupulosity OCD is not becoming more certain, more ethical, or more perfect.
It’s learning to stop responding to the doubt as if it needs to be solved.
This often feels counterintuitive at first—especially if you’re used to trying to “get it right.”
Exposure and Response Prevention (ERP)—the gold-standard treatment for OCD—focuses on changing your relationship to uncertainty.
This includes:
Reducing compulsions
Not confessing, not over-apologizing, not mentally reviewingAllowing uncertainty
Practicing responses like:
“Maybe I did something wrong. Maybe I didn’t.”Acting based on values, not fear
Making decisions without needing absolute certainty first
Over time, your brain learns something essential:
You don’t need certainty to move forward.
Who Experiences Scrupulosity OCD?
Scrupulosity often shows up in people who are:
Thoughtful and introspective
Highly responsible
Holding themselves to high internal standards
It can also become more intense during major life transitions.
We often see this during pregnancy and postpartum, when the pressure to be a “good” parent or make the “right” decisions feels especially high. Intrusive doubts about whether you are doing enough—or doing something wrong—can take on an obsessive, persistent quality.
A Final Thought
If this sounds familiar, it’s not because you’re a bad person.
It’s because your brain is over-sensitive to doubt—and keeps trying to solve something that can’t be solved by certainty.
Scrupulosity OCD is a treatable condition, not a reflection of who you are.
You don’t have to keep proving, over and over again, that you’re a good person.
You’re allowed to live your life without reaching a final answer.
Next Step
If you’re noticing this pattern, working with a therapist trained in OCD and ERP therapy can make a meaningful difference.
At Red Elm Psychotherapy, we specialize in treating OCD—including scrupulosity—using structured, evidence-based approaches designed to actually break the cycle.
Schedule a consultation to get started.
About the Author
Dr. Niles Cook is a licensed clinical psychologist and co-founder of Red Elm Psychotherapy. He specializes in the treatment of obsessive-compulsive disorder (OCD), including scrupulosity and other forms of intrusive doubt, using Exposure and Response Prevention (ERP).
Dr. Cook works with high-achieving adults and professionals who feel stuck in cycles of overthinking, uncertainty, and the need to get things exactly right. His approach is structured, direct, and grounded in evidence-based treatment.
He provides telehealth therapy across Virginia and is listed with the International OCD Foundation.
Relationship OCD: Why You Can’t Stop Doubting Your Relationship
Woman sitting on couch looking thoughtful while partner sits blurred in background, representing relationship doubt and overthinking
“What if I don’t actually love them?”
“What if I’m making a huge mistake?”
“Why am I constantly overanalyzing every single thing they say or do?”
Most people experience moments of doubt in a relationship. But for some, these questions don’t just pass—they loop. They intensify. They become a background noise that never truly shuts off, eventually taking over your daily life and your ability to enjoy your partner.
If your relationship feels less like a partnership and more like a puzzle you are desperately trying to "solve," you might be experiencing Relationship OCD (ROCD).
What Is Relationship OCD?
ROCD is a common subtype of Obsessive-Compulsive Disorder. It isn’t a sign that your relationship is "wrong" or that you’ve fallen out of love. Instead, it is a cycle driven by a low tolerance for uncertainty.
While everyone has fleeting doubts, someone with ROCD feels an urgent, crushing need for 100% certainty about their feelings, their partner’s flaws, or their long-term compatibility. Because perfect certainty is impossible to find, the brain stays stuck in a loop of searching for it.
Common Signs of ROCD
ROCD usually manifests through intrusive thoughts (obsessions) and the actions you take to quiet them (compulsions). You might find yourself:
Mentally Checking: Constantly asking yourself, "Do I feel 'the spark' right now?" while kissing or hanging out.
Comparing: Obsessively comparing your partner’s traits or your relationship to friends, exes, or even fictional characters.
Reassurance Seeking: Asking friends, family, or even your partner if you "seem" happy or if the relationship looks "right" to them.
Researching: Spending hours on forums or reading articles trying to find a definitive "sign" that you should stay or leave.
Hyper-fixating on Flaws: Becoming consumed by a partner’s physical "imperfections" or minor personality quirks as evidence that they aren't "The One."
Why It Feels So Real
The paradox of OCD is that it targets what you value most. If you didn’t care about your partner or the concept of love, your brain wouldn't bother using these thoughts to scare you.
Furthermore, ROCD exploits the fact that human emotions are naturally fluid. We don’t feel "madly in love" every second of every day. To an ROCD brain, a slight dip in affection isn't just a normal part of a Tuesday—it’s viewed as an emergency that must be analyzed immediately.
ROCD vs. Normal Doubt
How do you know if you're in the wrong relationship or if you just have OCD?
Normal Doubt
Comes and goes; usually triggered by specific, real-world issues.
Doesn't usually result in hours of "mental work" or research.
You can focus on other parts of your life (work, hobbies).
Feelings are generally stable despite the doubt.
Relationship OCD
Persistent, intrusive, and urgent.
Leads to repetitive compulsions to ease anxiety.
The doubt feels like a "cloud" over everything you do.
Feelings feel "gone" because anxiety is suppressing them.
The Cycle of ROCD
ROCD thrives on a specific loop:
The Trigger: A thought or feeling (e.g., “I didn’t miss them today”).
Anxiety: A spike of fear or "urgency" to figure out what that means.
Compulsion: You Google "signs of falling out of love" or check your feelings.
Temporary Relief: You feel better for a moment because you found an answer.
The Repeat: The doubt returns, and you need a stronger "fix."
There is a Way Out
The goal of therapy isn't to prove that your relationship is perfect—it’s to help you live comfortably with the fact that no relationship is certain.
Exposure and Response Prevention (ERP) is the gold standard for treating ROCD. It helps you break the cycle by teaching your brain that you don't have to "answer" every intrusive thought that pops into your head. You can learn to experience a doubt without letting it dictate your actions.
You don’t need to end your relationship to get relief, and you don’t need to reach 100% certainty before you start feeling better.
Take the Next Step
If this cycle feels familiar, you don’t have to keep trying to figure it out on your own. Our specialists are trained in evidence-based tools to help you reclaim your life from the "What Ifs."
Explore our Relationship OCD Service Page
Learn more about OCD Therapy
HowERP Therapyworks
You deserve to be present in your life, rather than stuck in your head.
About the Author
Dr. Niles Cook, PsyD is a licensed clinical psychologist and co-founder of Red Elm Psychotherapy. He specializes in the treatment of obsessive-compulsive disorder (OCD) and anxiety using Exposure and Response Prevention (ERP). Dr. Cook works with high-achieving adults and professionals who feel stuck in cycles of overthinking, doubt, and perfectionism. He provides telehealth therapy across Virginia. He is listed with the International OCD Foundation.
Why ERP Feels So Hard (And Why That Means It’s Working)
You know the thoughts don’t make sense—but they still feel urgent. This is why ERP feels so hard, and why that discomfort is actually part of getting better.
If you’re reading this, you probably already know that your intrusive thoughts don’t make sense. You know the logic is flawed. You know that checking the stove for the fifth time or replaying that conversation in your head won’t actually change the outcome.
Logic isn't the problem.
The problem is that these thoughts feel urgent, important, and impossible to ignore. They don't feel like "just thoughts"—they feel like fires that need to be put out right now.
The Loop You’re Stuck In
Most people try to think their way out of OCD. You analyze. You Google. You seek reassurance from your partner. You replay the "evidence" over and over.
And for a second, it works. The anxiety dips. You feel a brief moment of "certainty."
But then the doubt creeps back in. “But what if I missed something? What if this time is different?” This is the OCD cycle of Obsession → Compulsion → Temporary Relief. Every time you perform a compulsion to feel safe, you are accidentally teaching your brain that the "threat" was real. You are feeding the monster to keep it quiet, but the monster only gets hungrier.
Reclaiming Your Brain: What ERP Actually Is
Most clinical descriptions of Exposure and Response Prevention (ERP) make it sound like a chore. In reality, ERP is a rebellion. ERP is not about "getting rid of thoughts." (Spoiler: you can't control what pops into your head). It’s about changing your relationship to those thoughts. It means doing the exact opposite of what your brain is screaming at you to do.
What ERP Feels Like in Practice:
Letting a thought sit in your mind without trying to "answer" it or solve it.
Resisting the urge to check—whether that’s a door lock, a physical sensation, or a memory.
Staying in the discomfort of uncertainty instead of chasing the high of reassurance.
Why It Feels "Wrong"
Here is the truth that most textbooks won't tell you: Doing ERP feels irresponsible.
When you stop performing your compulsions, your brain will tell you that you’re being careless. It will tell you that you’re ignoring something dangerous. It will feel like you are walking a tightrope without a net.
That feeling? That’s the feeling of your brain re-wiring itself. If it feels "right" and comfortable, you aren't doing ERP. When it feels risky and uncertain, you are finally interrupting the cycle that has kept you stuck for years.
Is ERP Therapy Hard?
Because ERP is the "gold standard" for OCD treatment, people often ask if the process is as intense as it sounds. The short answer is: Yes, ERP is hard because it requires you to intentionally lean into uncertainty rather than running away from it.
However, "hard" doesn't mean "reckless." In our practice, we don't throw you into the deep end. We use a fear hierarchy to help you face challenges in a structured way. The goal isn't just to be "brave"—it’s to retrain your brain's alarm system so that eventually, the things that feel impossible today become background noise.
Stop Analyzing. Start Living.
OCD thrives on the "What If." ERP thrives on the "So What?" By leaning into the uncertainty, you stop being a prisoner to your own thoughts. You stop managing your anxiety and start living your life again.
By leaning into the uncertainty, you stop being a prisoner to your own thoughts. You stop managing your anxiety and start living your life again.
Dr. Niles Cook specializes in treating OCD using evidence-based Exposure and Response Prevention (ERP). He works with adults across the full spectrum of OCD presentations, helping them move past the "mental loops" and back into the driver’s seat.
If this feels familiar, you don’t have to keep managing it alone.
We offer evidence-based OCD treatment for adults across Virginia.
If you’re experiencing this during pregnancy or postpartum, you can learn more about our postpartum and perinatal therapy here.
Why Do Intrusive Thoughts Feel So Real Postpartum?
Intrusive thoughts after having a baby can feel frighteningly real. This post explains why postpartum intrusive thoughts happen, what they mean, and how to begin stepping out of the cycle.
One of the most distressing parts of postpartum intrusive thoughts isn’t just what they are—it’s how real they feel.
Many women experience intrusive thoughts after birth that feel confusing, unfamiliar, and deeply out of character. These thoughts often show up as sudden “what if” scenarios:
What if I drop the baby?
What if I lose control?
What if I accidentally hurt them without meaning to?
The mental strain of trying to understand or prevent these thoughts is often compounded by the realities of postpartum life—sleep deprivation, feeding challenges, physical recovery, relationship shifts, and caring for other children.
Why Do Postpartum Intrusive Thoughts Feel So Convincing?
Intrusive thoughts don’t just feel like random mental noise. They often feel like signals—something important, something meaningful, something you need to pay attention to.
This is a key feature of postpartum anxiety and postpartum OCD—the thoughts feel urgent and believable, even when they don’t reflect your intentions.
What’s Actually Happening in the Brain
When an intrusive thought appears, it can quickly activate the brain’s threat detection system.
Your brain automatically asks:
“Is this dangerous? Do I need to act?”
When a thought is flagged as even possibly important:
Attention locks onto it → it becomes hard to ignore
Anxiety increases → your body responds as if something is wrong
The thought feels meaningful → it no longer feels like “just a thought”
This is part of your brain’s built-in alarm system. Its job is to keep you and your baby safe—but it doesn’t distinguish well between a thought about harm and actual danger.
This same alarm process is a core feature of OCD, where intrusive thoughts become “sticky” because they’re treated as meaningful or threatening. You can read more about how this pattern works in the OCD cycle here.
Why Intrusive Thoughts Can Feel Stronger After Birth
The postpartum period is a time of increased vulnerability, responsibility, and change.
Your brain adapts by becoming more alert to potential threats:
You are caring for a completely dependent baby
The stakes feel high and constant
Your daily structure and identity are shifting
This heightened awareness is protective—but it also means your brain is:
More likely to scan for “what if” scenarios
Less able to dismiss unlikely thoughts
More reactive to uncertainty
At the same time, sleep deprivation and physical recovery can make it harder to step back from anxious thinking.
For many high-functioning women, there’s an added layer: you’re used to feeling capable and in control. Postpartum can feel unfamiliar and high-stakes, which makes intrusive thoughts feel even more unsettling and important.
What Intrusive Thoughts Actually Mean
Intrusive thoughts feel true because of how your brain responds to them—not because they reflect your intentions.
In fact, postpartum intrusive thoughts often target what you care about most.
The more you care about your baby’s safety
The more responsible you feel
The more seriously you take motherhood
…the more likely your brain is to generate distressing “what if” thoughts in those exact areas.
This is not a sign that you want something to happen.
It’s a sign that your brain is trying—imperfectly—to protect what matters most.
Intrusive thoughts target what you care about, not what you want.
When Intrusive Thoughts Become Postpartum OCD
For many women, the distress isn’t just the thoughts—it’s what follows.
You may find yourself:
Analyzing what the thought “means”
Checking your reactions
Avoiding certain situations
Seeking reassurance
Trying to suppress or neutralize the thought
These responses are completely understandable—but they can unintentionally reinforce the cycle.
Over time, this can develop into postpartum OCD, where the pattern looks like:
Intrusive thought → anxiety → attempt to control or get certainty → temporary relief → thought returns stronger
This cycle is common—and highly treatable with the right support.
You’re Not Alone—and This Is Treatable
If you’re experiencing intrusive thoughts during pregnancy or postpartum, you are not alone—and this does not mean something is wrong with you.
These thoughts are a reflection of a brain that is trying to protect, not harm.
With the right support, it’s possible to feel less caught in the cycle and more grounded in your role as a parent.
To learn more, explore our pages on perinatal OCD and ERP therapy for OCD.
If This Feels Familiar
If you’re noticing intrusive thoughts that feel hard to shake, you don’t have to navigate this alone.
Many women experience this in the postpartum period—and with the right support, it can become much more manageable.
If you’d like to learn more or see if working together feels like a good fit, you can contact Red Elm Psychotherapy to get started.
About the Author
Dr. Erin Cook is a clinical psychologist and co-founder of Red Elm Psychotherapy, a Virginia-based practice specializing in perinatal mental health and OCD. She works with women navigating pregnancy, postpartum, and early motherhood—especially when anxiety or intrusive thoughts feel overwhelming or out of character.
Her approach is thoughtful, collaborative, and grounded in helping clients feel less alone in what they’re experiencing.
Why OCD Feels Impossible to Stop: Understanding the Obsessive-Compulsive Cycle
Obsessive-Compulsive Disorder (OCD) traps people in a cycle of intrusive thoughts, anxiety, and compulsions. Learn how the OCD cycle works and how evidence-based treatment can help break it.
At Red Elm Psychotherapy, we specialize in helping people who feel trapped in the cycle of Obsessive-Compulsive Disorder (OCD).
Many people have heard of OCD, but the reality of living with it is often misunderstood.
OCD is not simply being organized or worrying too much. Instead, it involves a powerful cycle of intrusive thoughts and repetitive behaviors that can create intense anxiety, doubt, and mental exhaustion.
People with OCD often know that their fears may not make logical sense — but the anxiety and uncertainty feel so overwhelming that it becomes incredibly difficult to ignore the urge to act.
Understanding how this cycle works is the first step toward breaking it.
What is Obsessive-Compulsive Disorder?
OCD has two core components: obsessions and compulsions.
Obsessions
Obsessions are intrusive thoughts, images, or urges that suddenly enter a person’s mind and cause distress.
These thoughts often feel disturbing or out of character. Most people with OCD recognize that the thoughts do not reflect who they truly are — but the uncertainty they create can feel impossible to tolerate.
Common themes for obsessions include:
Contamination: Fear of germs, dirt, or becoming sick.
Safety/Harm: Fear of causing harm to oneself or others, or fear of bad things happening (this is common in Perinatal OCD).
Symmetry/Order: A need for things to be "just right" or balanced.
Relationship Doubts: Persistent, intrusive uncertainty about a partner’s "rightness" or your own feelings, often called Relationship OCD (ROCD).
Moral or Religious Certainty: Known as Scrupulosity, this involves intrusive thoughts that feel like moral failings or "unacceptable" religious or aggressive thoughts that are inconsistent with your true values.
Compulsions
Compulsions are behaviors or mental rituals that someone feels driven to perform in order to reduce the anxiety created by the obsession.
These behaviors may be visible, such as checking or washing, or internal, such as mentally reviewing memories or repeating phrases in one’s mind.
Compulsions may bring temporary relief, but they also strengthen the OCD cycle.
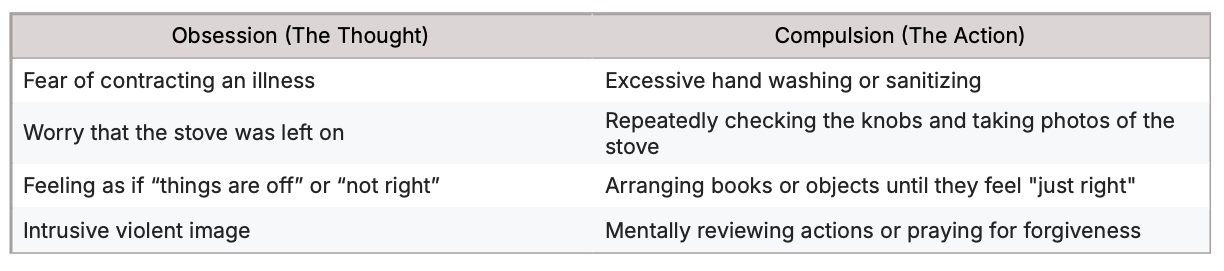
Common Examples of Obsessions and Compulsions
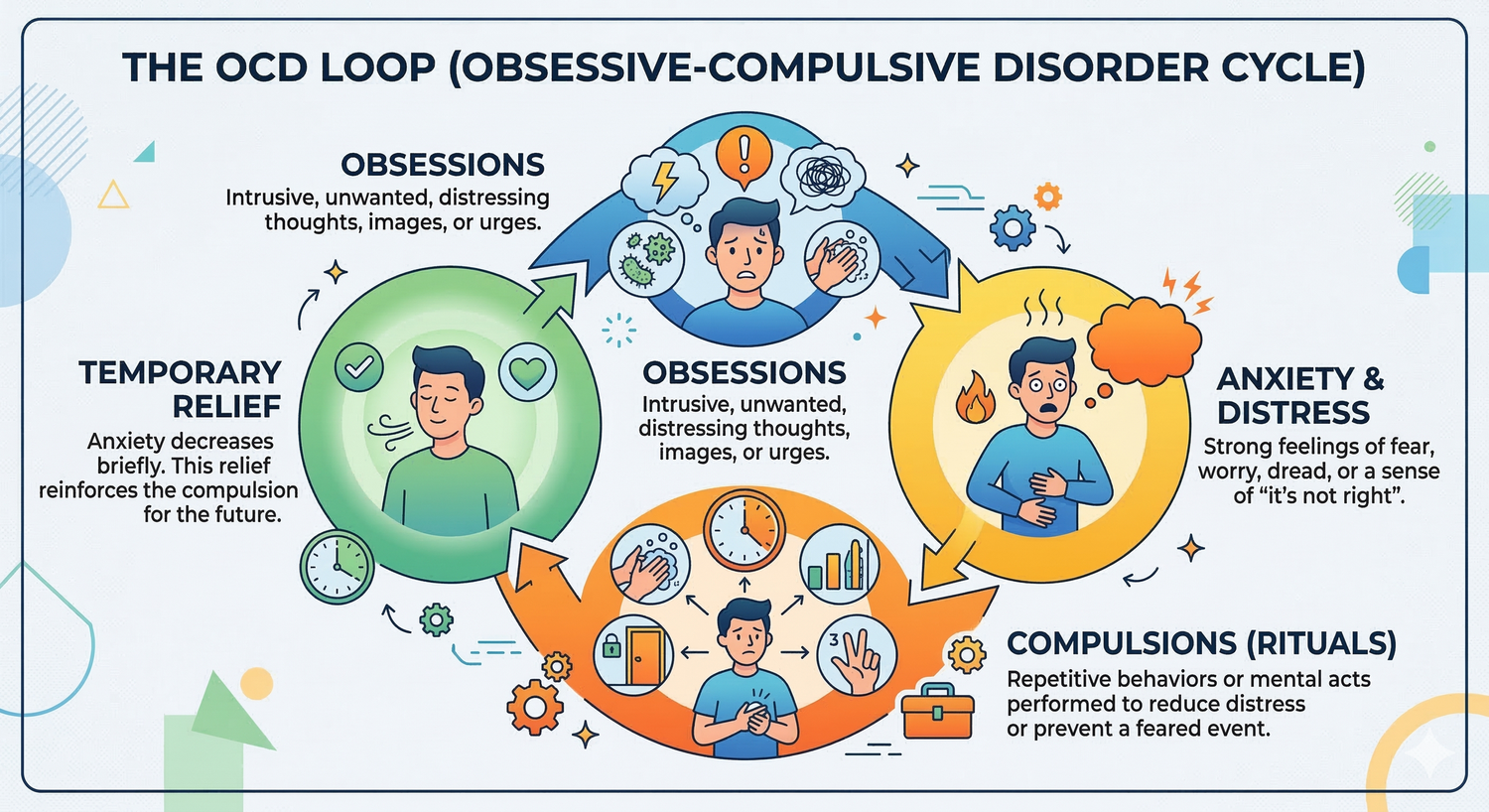
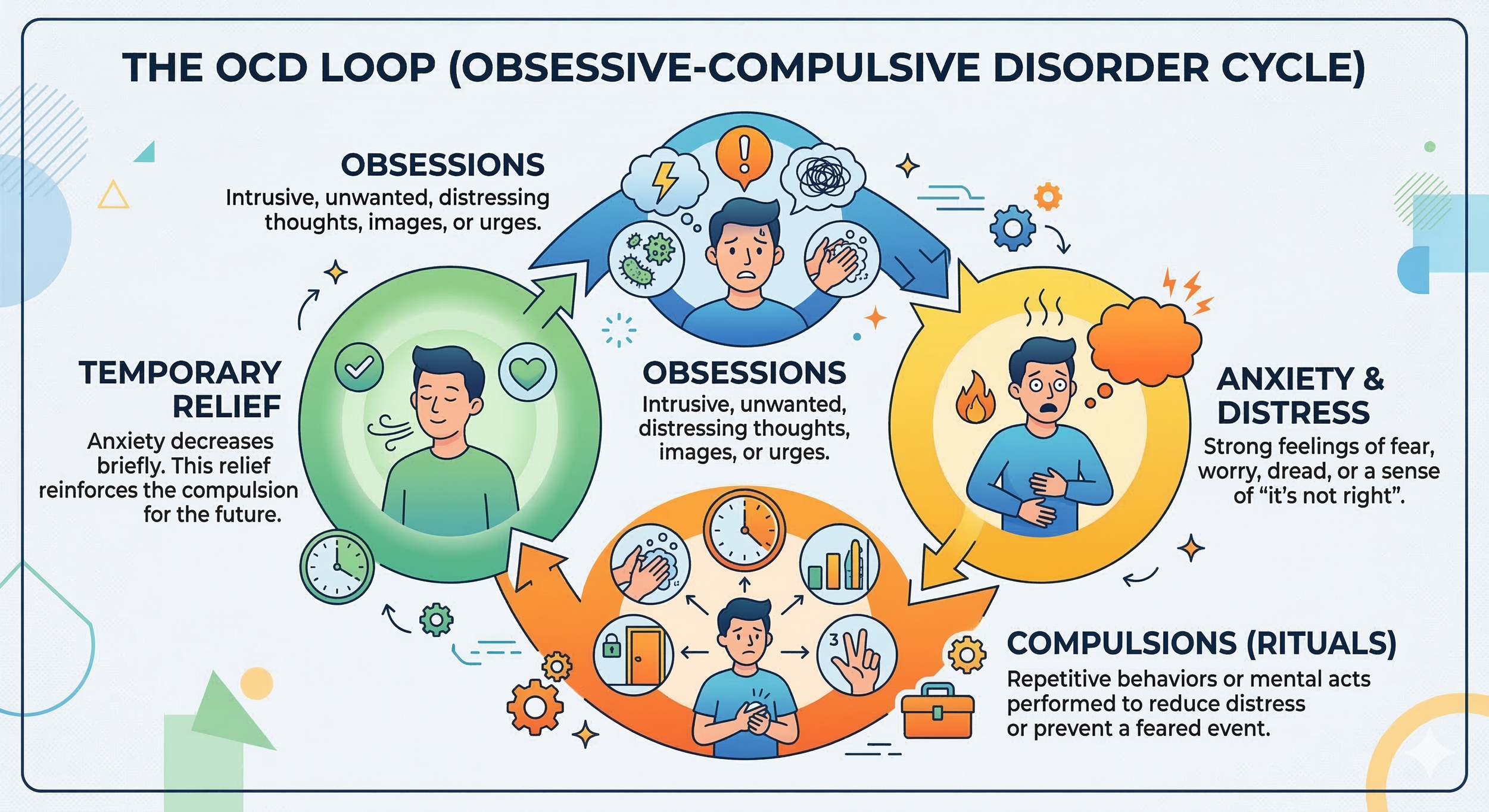
What is the OCD Cycle?
At its core, the OCD cycle is a self-reinforcing loop that keeps the brain stuck in a state of high alarm. Understanding these four stages is the first step toward breaking the pattern:
Obsession (The Trigger): An unwanted, persistent thought pops into the mind (e.g., “What if I left the stove on?”).
Anxiety (The Reaction): The obsession causes a surge of extreme fear and distress. You feel an urgent need to act to prevent a disaster.
Compulsion (The Safety Behavior): To reduce the immediate anxiety, you perform a repetitive behavioral or mental act (e.g., checking the stove).
Temporary Relief (The Payoff): Performing the compulsion provides a brief reduction in anxiety.
The Reinforcement Trap: Because the anxiety drops after the behavior, your brain mistakenly learns that the compulsion prevented the feared outcome. This "negative reinforcement" is why the cycle is so hard to stop without specialized support like ERPTherapy. In fact, even when you logically know the cycle is a 'trap,' it can still feel impossible to break. Read more about why insight alone isn't enough to stop the OCD loop.
The cycle is relentless because the compulsion provides relief, which trains the brain to rely on the ritual, keeping the person trapped between their obsession and their anxiety.
Example of the OCD Cycle in Daily Life
Sarah reaches for her car keys, ready to start her day, when a sudden image of her kitchen in flames flashes across her mind.
The thought isn't just a passing worry; it triggers an immediate surge of anxiety, causing her heart to race and her stomach to knot with a physical sense of dread. She feels an urgent need to "fix" the uncertainty before something catastrophic happens.
To quiet the alarm bells in her head, Sarah retreats to the kitchen to perform a compulsion. She doesn't just look at the machine; she stares at the unplugged cord and taps the power button exactly three times to ensure there is no residual electricity.
This ritual provides a wave of temporary relief, a brief moment where the anxiety dissipates and she feels she has successfully averted a disaster. But the relief comes at a cost.
Sarah’s brain learns (incorrectly) that her checking and tapping prevented the disaster, making the urge to repeat the compulsion even stronger the next time she leaves the house.
Who is Vulnerable to OCD?
Late Adolescence/Early adulthood
The amount of change, both biologically as well as socially, that occurs during this age period make this population particularly vulnerable to OCD. Almost 80% of all cases start to exhibit symptoms before the age of 24.
Women, especially during pregnancy and the postpartum period
The occurrence of intrusive thoughts as well as full OCD is quite prevalent in this population due to uniquely high hormonal fluctuation. Pregnancy makes a person twice as likely to develop OCD than those not pregnant.
Individuals in both highly competitive and high performing fields often mistake “perfectionism” and “single-mindedness” for latent anxiety and OCD tendencies. While there has not been a causal relationship found between stress and OCD, there is a disproportionately large representation of high performers who have OCD.
Individuals with other mental health disorders
People who struggle with Tourettes and/or Tic disorders, Anxiety disorders, Depressive disorders, as well as ADHD have higher rates of OCD than those who do not.
Effective Treatment for OCD
The good news is that OCD is highly treatable.
The most effective therapy for OCD is a specialized form of cognitive behavioral therapy called Exposure and Response Prevention.
ERP works by gradually helping individuals face the thoughts or situations that trigger anxiety while learning to resist the compulsive behaviors that maintain the cycle.
Over time, the brain learns something new:
The intrusive thought is not dangerous, and the compulsion is not necessary.
As this learning occurs, anxiety decreases and the cycle of OCD begins to weaken.
This will be discussed in more detail in our next blog post
Getting Help
Living with OCD can feel exhausting and isolating, but effective help IS available.
At Red Elm Psychotherapy, we provide evidence-based treatment for OCD and anxiety disorders using Exposure and Response Prevention.
If you or a loved one is struggling with the relentless cycle of OCD, you can contact our practice here to schedule a consultation. Our clinic offers personalized, evidence-based treatment plans designed to help you regain control of your life.
About the Author
Niles Cook, PsyD, is a clinical psychologist specializing in the treatment of obsessive-compulsive disorder (OCD) and anxiety disorders using Exposure and Response Prevention (ERP). He provides evidence-based therapy for adults experiencing intrusive thoughts, compulsive behaviors, and anxiety. He practices at Red Elm Psychotherapy in Virginia.
Is It Normal to Have Intrusive Thoughts About Harming Your Baby?
Many new mothers experience frightening intrusive thoughts after their baby is born. These thoughts can feel disturbing and isolating, but they are far more common than most women realize. Learn why these thoughts happen, when they are normal, and when they may be part of postpartum OCD.
Postpartum Intrusive Thoughts, Anxiety, and OCD—What’s Normal and What’s Not
If you’ve had a sudden, disturbing thought about harming your baby, you are not alone—and it does not mean you want to act on it. In fact, these thoughts are far more common than most people realize.
Many women are surprised by the kinds of intrusive thoughts that can show up after a baby is born.
Sudden images of their baby being hurt.
Fears that their baby might fall, get sick, or stop breathing.
Thoughts about accidentally harming their baby while caring for them.
Or frightening thoughts about causing harm themselves.
These experiences can take many forms, but they often center around a baby’s safety.
For many mothers, these thoughts feel deeply disturbing and isolating—like you’re the only person who has ever experienced something like this.
While fears about the baby are most common, postpartum OCD can also show up as:
Intense doubts about your partner or your relationship (Relationship OCD).
Severe guilt or fears about being an "immoral" person (Scrupulosity).
Sudden images of the baby being hurt or falling.
Are Intrusive Thoughts After Baby Normal?
In reality, intrusive thoughts in the postpartum period are extremely common. In a large study from Canada, researchers found that 95% of new mothers had thoughts about their baby being accidentally harmed, and more than half had thoughts about harming their baby themselves.
These experiences are intrusive, meaning they appear suddenly and feel unwanted or upsetting. Mothers who experience them are usually frightened by them and wish they would go away.
Many mothers tell me the most frightening part isn’t the thought itself, but the fear that having the thought might mean something about who they are as a mother.
Having these thoughts does not mean that you will harm your baby.
In fact, the opposite is often true. Mothers who experience these thoughts are often deeply concerned about their baby’s safety and may be working very hard to prevent anything bad from happening.
The fact that the thoughts feel upsetting or frightening is often a sign that you care deeply about keeping your baby safe.
Intrusive thoughts in postpartum anxiety and OCD are very different from the rare condition postpartum psychosis. In OCD, the thoughts feel unwanted and frightening, and mothers are typically trying very hard to prevent anything bad from happening.
Why Do These Thoughts Happen?
After birth, a mother’s brain undergoes major shifts.
Your brain becomes much more sensitive to potential threats. Hormones strengthen your bond with your baby, but they also heighten vigilance around your baby’s safety.
At the same time, your brain begins to simulate possible danger scenarios.
In many ways this makes sense. Protecting your baby becomes one of your brain’s most important priorities during this period.
But when these changes combine with sleep deprivation, feeding challenges, birth trauma, physical recovery, relationship changes, high-risk pregnancies, pregnancy after loss, medically complex babies, or pelvic floor injuries, these thoughts can begin to feel overwhelming.
Many mothers naturally try to push these thoughts away or analyze what they might mean. Unfortunately, both of these strategies can make the thoughts come back even more strongly.
Sometimes they also start to feel sticky.
When Intrusive Thoughts May Be Postpartum OCD
For some mothers, these thoughts begin to get stuck.
Instead of coming and going, they start to trigger intense anxiety and feel harder to dismiss. When this happens, the thoughts may be part of a larger pattern called perinatal OCD.
A sudden thought like:
“What if I drop my baby down the stairs?”
can feel incredibly distressing.
In response, a mother might begin avoiding situations that trigger the thought — for example avoiding carrying her baby on the stairs altogether.
Many mothers also begin avoiding everyday caregiving situations where these thoughts tend to appear: walking on stairs, bathing the baby, feeding them, or holding them near balconies or sharp objects.
If avoidance isn’t possible, she may try to manage the anxiety in other ways. She might count each step as she walks down the stairs, repeat reassuring phrases in her mind, or mentally check whether she feels “in control.”
While these strategies may reduce anxiety in the moment, they unintentionally teach the brain that the thought was dangerous and needed to be controlled.
Over time, the cycle reinforces itself.
How Treatment Helps
The most effective treatment for OCD is Exposure and Response Prevention (ERP).
ERP helps mothers gradually face the situations that trigger their fears while learning to stop the avoidance, reassurance seeking, and rituals that keep anxiety stuck.
For example, treatment might involve gradually practicing carrying your baby on the stairs again while learning not to rely on counting, reassurance, or other rituals to reduce anxiety.
Over time, the brain learns something new: these thoughts are not dangerous and do not need to be controlled.
ERP is highly effective, and it is safe for both mothers and their babies.
With the right support, many mothers recover fully from postpartum OCD and are able to enjoy their babies and their lives again.
If You're Struggling
If intrusive thoughts have started to feel overwhelming or are taking away from the joy of early parenthood, you are not alone.
Support can help. Our clinic specializes in postpartum and perinatal therapy with an emphasis on perinatal OCD and anxiety, and we work with mothers who are experiencing exactly these kinds of thoughts.